I have made very clear in recent posts that one negative feature of the tax bill, increasing national debt by $1 trillion over ten years, greatly outweighs its good features. For this reason I ask Nebraska Senator Deb Fischer to put the welfare of our country ahead of the demands of her Republican colleagues and vote against the bill.

Nevertheless, the tax bill does have beneficial features and I would like to acknowledge them here. Major ones are:
- Lowering the corporate tax rate from 35% to 21% and moving to a territorial system, making us far more internationally competitive and encouraging our multinational corporations to bring their foreign profits back home.
- Establishing immediate expensing of capital investment, thereby speeding up business investment and increasing economic growth.
- Reducing itemized deductions for state and local taxes and mortgage interest, but not eliminating them as should be done for much greater revenue savings.
- Increasing the standard deduction to $12,000/$24,000 (for singles/couples) which will reduce the number of individual taxpayers who itemize deductions from 30% to just 6%. This single feature alone achieves major simplification.
- Measuring inflation adjustments for income thresholds by the Chained Consumer Price Index (CCPI) rather than the current CPI. CCPI takes consumer behavior into account when computing inflation and will lead to an increase in tax revenue over time.
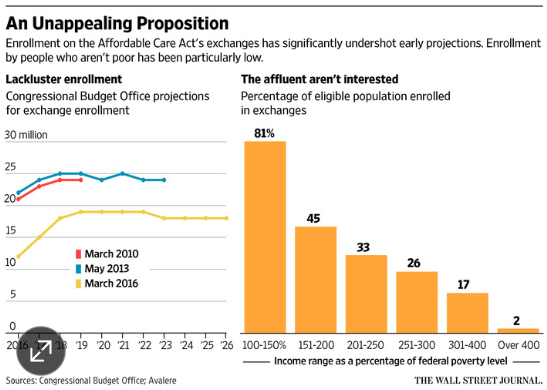
- Eliminating the individual mandate for the ACA which will lead to fewer healthy people signing up for health insurance. This begins a process of healthcare cost reform which must continue much further to significantly reduce the cost of American healthcare. Much more later.
Conclusion. The good features in the tax bill do not nearly outweigh the awfulness of adding $1 trillion to our debt over the next ten years. The Republican Party should be ashamed of itself for such poor fiscal and economic stewardship. What is it thinking?